KEY
FACTS
TECHNIQUE
Surgical removal of the implants
INTERVENTION TIME
1,5-2,5 hours
PAIN
3 (Scale 1-10)
DOWNTIME
3-5 days
RESULT
Immediate effect, final result after 2-3 months
COSTS
Beast Implant Illness+Capsulectomy from € 8,500 Initial consultation for new patients: € 70
PAYMENT
Advance bank transfer, cash or card payment possible.


Breast Implant Illness
DO YOU WANT A RETURN TO BEAUTIFUL BREASTS WITHOUT SYMPTOMS AND PAIN?
For most patients, breast augmentation is accompanied by an increased, positive body image – in rare cases, however, the implants can lead to inexplicable symptoms such as hair loss, headaches, sleep disorders, muscle pain, or other symptoms. For these unfortunately very unspecific symptoms, the term “Breast Implant Illness” has been established for many years. Since these are non-specific symptoms, they should also correlate with the time a few weeks or months after the breast operation, so that one can think of a diagnosis of “Breast Implant Illness”.
Breast implant illness does not refer to symptoms that are directly related to breast surgery with implants. It is a collective term for conditions that have been observed in close temporal proximity. This does not mean that there is a causal connection, but at present this cannot be ruled out across the board. Clarifying this connection is a major, sensitive topic and is currently being researched.
WHAT HAPPENS BEFORE THE OPERATION.
After an in-depth consultation and analysis, we recommend the complete removal of the breast implants if Breast Implant Illness is suspected, as we have observed a disappearance of the symptoms in almost all patients.
WHAT HAPPENS DURING THE OPERATION.
Capsulectomy vs en bloc removal.
Patients who come to us with this disease have already dealt intensively with the topic and often want the “en-bloc” removal of the implants, which is often mentioned in internet forums. In this case, not only the implants but also the capsule surrounding them should be removed without leaving any residue. We do our best during the operation to remove all easily accessible parts of the capsule – however, in the case of implants that lie under the muscle, the capsule is usually also firmly fused with the rib muscles and the bony ribs, and removal of these segments can lead to a so-called “pneumothorax” (= accumulation of air in the lungs), which has fatal consequences. Therefore, in every Breast Implant Illness case we perform a removal of the implants as well as a capsulectomy (= the removal of the capsule parts) – however, we refrain from the forced removal of firmly grown tissue because of the risks. The list of patients in whom a small proportion of the firmly grown capsule remains and who have become symptom-free again despite this fact is long and we are therefore convinced that the stubborn attempt to always remove “en bloc” is not correct. Especially in patients who do not have capsular fibrosis, but only a very thin capsule, a total en bloc removal is not always possible or necessary.
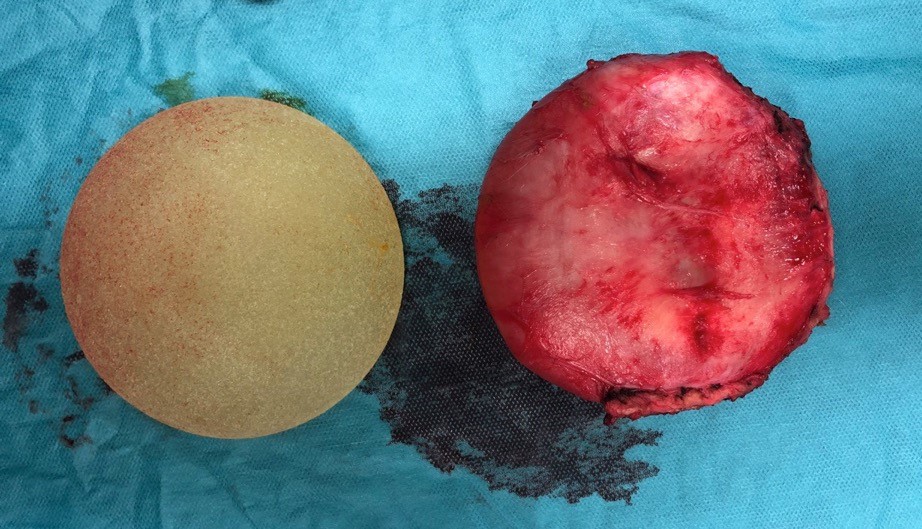
During the procedure we document exactly how the cavity looked before and after removal and which part of the capsule we removed and how. The implants are the property of the patient and are handed over to her.
WHAT HAPPENS AFTER THE OPERATION.
The operation takes place in Vienna in a day clinic and under general anaesthesia. An overnight stay in hospital is rarely necessary nowadays for medical reasons. Our patients are very happy to stay overnight if the journey is long or if you simply want a night’s rest from everyday life. When you are discharged, you will be given a support bra to wear for 6 weeks. You can reach my team and me at any time if you have any questions. You can always reach me on my mobile number after the operation, even at night.
Further check-ups in the surgery are important in order to optimally accompany the healing process. After 2-3 days the plaster is changed and after about 2 weeks the stitches are removed. Until the stitches are removed, you should avoid sport and do not get the stitches wet.
Result: A breast without implant and a new, better body feeling without symptoms.
Testimonials


Autologous fat can be an alternative to implants. In some cases, the wish to have implants removed is not a problem. I became aware of Dr. Bartsch through a Facebook group and felt very well taken care of right from the start. He took my symptoms seriously, advised me in detail, and then we made an appointment to remove the implants including the capsule. I wanted a video of the operation, which he also did. Since then, my symptoms have completely disappeared and I finally feel comfortable in my skin again! Thanks again to the whole team, I can only recommend theaesthetics.breast augmentation also possible with own fat. However, if you want to gain more than one cup size, you are better off with implants. Both the breast shape and sufficient body fat must be present.
FIRST CONSULTATION
You can reach us for an appointment for an initial consultation in several ways:
The ordination by phone: +4313535555
The ordination by mail: [email protected] or via the Contact form
Dr. Rolf Bartsch personally via Messenger: +4369911222000
FIRST CONSULTATION
You can reach us for an appointment for an initial consultation in several ways:
The ordination by phone: +4313535555
The ordination by mail: [email protected] or via the Contact form
Dr. Rolf Bartsch personally via Messenger: +4369911222000
The most important questions and answers
I am a specialist in plastic, aesthetic and reconstructive surgery and have been self-employed in this field for over 15 years. We do not have any contracts with health insurance companies – however, we can prepare applications for cost coverage in case of an existing supplementary insurance. Plastic surgeons in private practice in Austria hardly ever have contracts with health insurance companies. Should one plan an explantation via health insurance, a plastic surgery department in a public hospital is a possibility.
Since I have been working in this field for more than 15 years, I have performed about 100 “En-bloc” removals so far. This technique is not only used for Breast Implant Illness, but also for a complication that can occur after breast augmentation – the so-called capsular fibrosis – which is still a very frequently used technique.
Since our patients are increasingly requesting photo documentation of their “en bloc” removal, I also have photos and videos of procedures that have already been performed.
This is how we proceed: every seroma that is present is sent in and examined. BIA-ALCL is nevertheless a rare disease. If BIA-ALCL is suspected due to persistent swelling of the breasts on one or both sides or an accumulation of fluid around the implant, we can organize a CD30 test for our patients at the University Hospital in Graz. The pathology department in Graz is specialized in this examination.
If there is an existing rupture of the breast implant, it is completely removed and the pocket is thoroughly rinsed several times and then cleaned. Ultrasound examination of the lymph nodes is indicated only if symptoms persist postoperatively. Removal of the lymph nodes is only necessary in the case of confirmed BIA-ALCL, and is performed by gynecologists who specialize in this area.
Ultrasound for the diagnosis of a rupture is unfortunately often not sufficient. An ultrasound examination can show both a false positive result, i.e. a rupture although none is present, and a false negative result. In this case, a rupture would have been present but not visible on ultrasound. Therefore, we always recommend an MRI examination of the breasts if a rupture is suspected.
The pocket contaminated by a rupture of the breast implant is rinsed and cleaned several times with a Betaisodona solution (containing iodine). The antiseptic effect of this solution thus ensures that microorganisms and silicone particles are removed.
Since our patients increasingly request photo documentation of their “en bloc” removal, I also have photos and videos of procedures that have already been performed. We can document steps of the surgery by photo and video upon request.
If there are reasonable grounds for suspicion, we can send in the implants and have them pathologically examined. In any case, you will get your implants well packed after the operation to take home, since they are also your property.
If you wish, we will be happy to provide you with a copy of the surgical report, the intraoperative imaging material and the findings of any tests that may have been performed. You always have the right to be given your patient file, so this does not need to be discussed beforehand.
Drains are usually not necessary for (en-bloc) implant removal. However, if heavy bleeding unexpectedly manifests itself intraoperatively, we will resort to drains – these usually remain in the breast for one day, and are removed by me personally at the first follow-up appointment.
Signs of postoperative infection are pain and redness/heating of the breast or scar. Seromas or hematomas are manifested by a marked swelling of the entire breast and the breast feels hard. Usually, hematomas occur only on one side. If any of these symptoms occur, you can reach me at any time by phone (even at night) at my private cell phone number (+43 699 11222000).
We will give you a one-time dose of antibiotic through the vein during the surgery. In some cases, you will receive a prescription for an antibiotic, which you should take for a few days after the surgery.
If the implants are infected with mold, we will take a swab intraoperatively to identify the exact pathogen and then start appropriate therapy. Cases with mold infestation of the implants are in principle very rare.
We will have 3-5 scheduled check-ups: one the day immediately after implant removal to change the patches, in some cases another in about 4-5 days after the procedure, one after about 2 weeks for suture removal, then 6 weeks after surgery, and then the final check-up will be about 3 months after the procedure. If you have any questions or complaints, you can of course make an appointment with us in the office at any time. Personally, I can also be reached at +4369911222000 via Messenger.
Access is usually through the underbust crease. In some cases, we have also performed a breast lift in the same procedure, which naturally results in new scars. In principle, in revision surgery after breast augmentation, the access is usually chosen via the inframammary fold. Regardless of whether the procedure was chosen via the areola, via the axilla or primarily via the inframammary fold.
We found this point very exciting. As mentioned above, you have rights to all documents that we create before, during and after treatment. Therefore, we can only agree. If you do not have a “good gut feeling”, choose another doctor.
Our anesthesiologists will perform the anesthesia by laryngeal mask – the drugs used are usually a mixture of Propofol (=anesthetic) + Ultiva (=painkiller). The main side effects include a rapid drop in blood pressure with propofol (so it is injected very slowly), and respiratory depression with Ultiva. However, we are a very well-rehearsed team with our anesthesiologists, and their experience in the field is responsible for the fact that most patients come out of surgery almost pain-free, and are able to leave the hospital just a few hours after the procedure.
You can also see how anesthesia works in our clinic in this video: https://youtu.be/ei6H6IjltCc
You will be given a single dose of ceftriaxone during surgery – this is a broad-spectrum antibiotic that has a wide antibacterial spectrum to cover the most important germs. If there are any special allergies or diseases, we will adjust the antibiotic administration accordingly.
You will, of course, also receive an anti-nausea and pain medication intraoperatively through the peripheral venous catheter.
Smaller hemorrhages (from mostly very fine vessels) are cauterized during surgery using special electric forceps. Larger arterial hemorrhages are very rare – if a large vessel is injured, its opening can be sutured with a thread to stop the bleeding.
We will not use permanent foreign bodies in “en bloc” removal.
Already before the beginning of the surgery you will receive painkillers. During the surgery, our anesthesiologists will give you “Ultiva” – this is a strong, very short-acting opioid that is effective against the pain during the surgery and for a few hours afterwards. You will then be given a prescription for pain medication. You can take this painkiller up to 3 times a day if needed.
We always say: “your gut feeling must be right”. Let your instinct be your guide. But there are also a few hard facts that can make a possible decision easier for you:
- Experience: more than 2,800 breast procedures in the last 13 years.
- Safety: through a professional team, anaesthesia outpatient clinic and a specialised clinic
- Availability: Dr. Rolf Bartsch is available 24 hours a day via messenger at +4369911222000
- Technique: Surgery planning by means of 3D scan
- Innovation: Dr. Bartsch is a trainer for breast surgery at the European College of Aesthetic Medicine & Surgery and a speaker at international congresses.